Brooke Jasper was taking opioids every hour or two at the height of her drug addiction.
The Yorkton, Sask., woman lost custody of her kids and ended up homeless in Regina, all precipitated by an abusive relationship, she said.
“Some days I went without eating. Some days I was having trouble finding somewhere to sleep,” said the now-31-year-old.
Still, she considers herself lucky.
Last year, 421 deaths in Saskatchewan were confirmed or suspected to be from drug overdoses, making it the deadliest year on record, according to the Saskatchewan Coroners Service.
Jasper said she’s had Naloxone, a treatment that temporarily reverses the effects of an opioid overdose, administered on her between 50 and 100 times.
Once, Jasper said, it took 21 doses to bring her back when she took what she thought was fentanyl, an opioid responsible for 127 of Saskatchewan’s overdose deaths last year.
It turned out the drug contained carfentanil, which is even more deadly than fentanyl, she said.
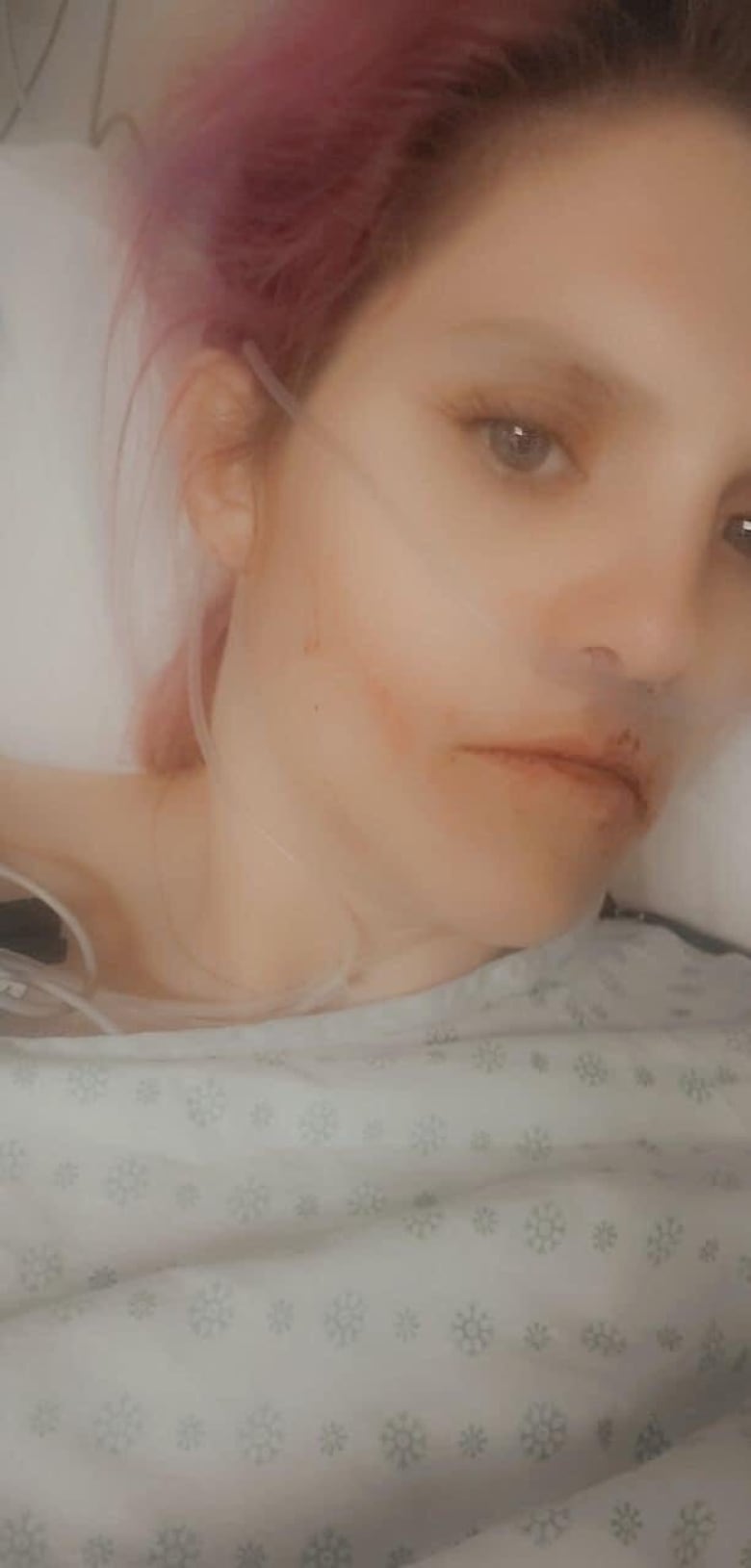
Now three months sober, Jasper said the province’s current opioid and overdose crisis is even worse for people living in rural Saskatchewan and smaller centres.
“I’m from Yorkton and there’s nothing here,” said Jasper.
Jasper said she waited a year after a stint in detox to get a bed at St. Joseph’s treatment centre in Estevan.
“If I didn’t have a ride to Regina detox or St. Joseph’s treatment centre then I wouldn’t have been able to go, and for the people here who don’t have rides where do they go?” Jasper said.
“They don’t go anywhere. There’s nothing. There’s no detoxes there’s no treatment centres.”
Drugs, on the other hand, are readily available in these smaller centres, according to Jasper.
“A lot of my friends were doing it. You could just walk uptown and find it.”
Chief Coroner Clive Weighill recently made recommendations to the Saskatchewan Health Authority that anyone who wants an addictions bed should have immediate access to one.
“Once they leave we know they will probably revert back to the lifestyle they were in and they won’t come back again,” Weighill told CBC’s Blue Sky.
“I think it’s really important for someone to have that option immediately and not be on a waiting list.”
Blue Sky41:31Saskatchewan’s fentanyl crisis: what’s the best way of preventing opioid overdoses and poisonings?
There’s a killer in Saskatchewan it’s called fentanyl. This synthetic drug is said to be 50 times stronger than heroin and it has proven to be lethal. The rise of fentanyl is just the latest development in an opioid addiction crisis that has been brewing for years. Last year drug overdoses claimed 421 lives in this province. Many of those deaths can be considered accidental as the people didn’t know what was in their drugs. Today we spoke with people who have first hand experience with addiction and overdose. We are grateful to everyone who shared their stories, it all helps fight stigma around drug use and addiction.
The province did not immediately respond to CBC’s requests for information about its plans to deal with the opioid crisis, or the wait times to find a space in detox and rehabilitation centers.
Colleen Larocque, who lives in Langenburg, said her 29-year-old son Mitchell Sveinbjornson died in 2020 after taking what he thought was cocaine.
It actually contained fentanyl and carfentanil, she said.
Larocque said everyone that took drugs with her son that night went to sleep, but Sveinbjornson never woke up.
“We’re losing first time users. It’s not just people who use every day. It’s not just people who use on the weekend who go to a party. We’re losing kids who have tried it for the first time because they don’t know what they are buying. We need to get the education in the schools,” Larocque said.
Like Jasper, Larocque said it’s worse for people living in rural areas.
“It’s not easy. Most of our supports are online.”
Larocque said people living in rural areas don’t have adequate access to testing strips, which would show the presence of fentanyl in drugs like the ones that killed her son.
They can’t wait six months. They can’t wait six weeks. They can’t wait six days.– Colleen Laroque
She also said Naloxone kits aren’t as accessible to people living in rural areas.
“There’s not enough detox beds. There’s not enough rehab beds. When somebody decides they want to go to rehab they want to go today. They can’t wait six months, they can’t wait six weeks, they can’t wait six days.”
100 per cent of drugs testing positive for fentanyl: PHR
Kayla DeMong, executive director of Prairie Harm Reduction, a safe consumption site in Saskatoon, said drug users at her centre have access to testing strips that show the presence of fentanyl or benzodiazepine.
“The root cause is toxic drug supply,” DeMong said. “Right now 100 per cent of everything we are testing is coming back positive for fentanyl.
“So whether it be somebody thinking they’re using cocaine or crystal meth, it’s all coming back positive for fentanyl.”
DeMong also said the province desperately needs immediate access to detox beds as well as more mental health supports and housing.













Leave a comment