It feels like everyone knows someone who has Omicron.
Maybe you got it, or your friend did. Perhaps your workplace is in an outbreak. Or you saw on the news that yet another celebrity or athlete or politician tested positive.
There’s this growing sense that catching the Omicron variant of the coronavirus is inevitable, perhaps even welcome — as if, after two years of collective anxiety over getting infected, we can all just get it over with and earn some hard-won immunity.
But, like everything with COVID-19, the reality is more complicated.
Multiple medical experts who spoke to CBC News — including infectious diseases specialists, virologists and epidemiologists — stressed that while getting infected with the virus is far more likely now, it’s still worth striving to avoid or, at the very least, delay.
“The dangerous temptation is to just let Omicron burn through populations while trying to jack up vaccination coverage,” said Dr. David Naylor, who led the federal inquiry into the 2003 SARS epidemic and co-chairs the federal government’s COVID-19 Immunity Task Force.
That’s because there are massive societal benefits to limiting the number of infections that pile up all at once — reducing pressure on a stretched-thin hospital system, for one thing — and huge costs if we don’t. Already, hospitalizations are surging to new heights, staff shortages are hitting various industries and an untold number of Canadians may wind up with serious infections or long-term health impacts.
This Omicron wave will certainly help boost immunity, “but at a potentially very high cost,” said Angela Rasmussen, a virologist at the Vaccine and Infectious Disease Organization at the University of Saskatchewan in Saskatoon.
This could even be the “last great push” toward the virus becoming endemic, said Raywat Deonandan, an epidemiologist and associate professor at the University of Ottawa, referring to when a threat like SARS-CoV-2 keeps circulating, but at a manageable baseline level.
“And there are people who are saying that’s a good thing,” he said. “It’s not a good thing to get there at this price.”
The Omicron variant has dealt hospitals a double blow — surging numbers of patients and plummeting levels of staff due to illness and isolation requirements. 2:44
Immunity boost a ‘silver lining’
Knowing just how many people are getting infected with Omicron is tough to determine, since limited access to official PCR testing in much of the country is muddying our data.
We’re surely missing tens of thousands of new cases, but even the reported figure — a country-wide seven-day average of more than 40,000 daily infections — is at a sobering, unprecedented high.
The Omicron variant, thankfully, is linked to less severe illness than its dominant predecessor, Delta, particularly for those who have the added protection of at least two vaccine doses. Yet it’s also more capable of evading immunity through both previous infection and vaccination, allowing it to tear through care homes, hospitals and households at a rate likely closer to measles than the original virus.
The usual numbers game means some of those being infected are winding up seriously ill — including an uptick in young children, who aren’t yet vaccinated — and a smaller percentage of a massive number of total cases is bad news for both overstretched hospital teams and all those who need that level of medical care.

The “silver lining” to the variant’s rapid spread is that the bulk of those infected will recover and gain an immunity boost in the process, particularly if they’re also vaccinated, said Dr. Dominik Mertz, an infectious diseases specialist with McMaster University in Hamilton.
“And this process is just much faster, with a variant that spreads so quickly, versus one where you might be more able to slow it down,” he said. “But if this wave lasts for weeks and weeks, many health-care systems could be overwhelmed. “And that’s really the concern at this point of time.”
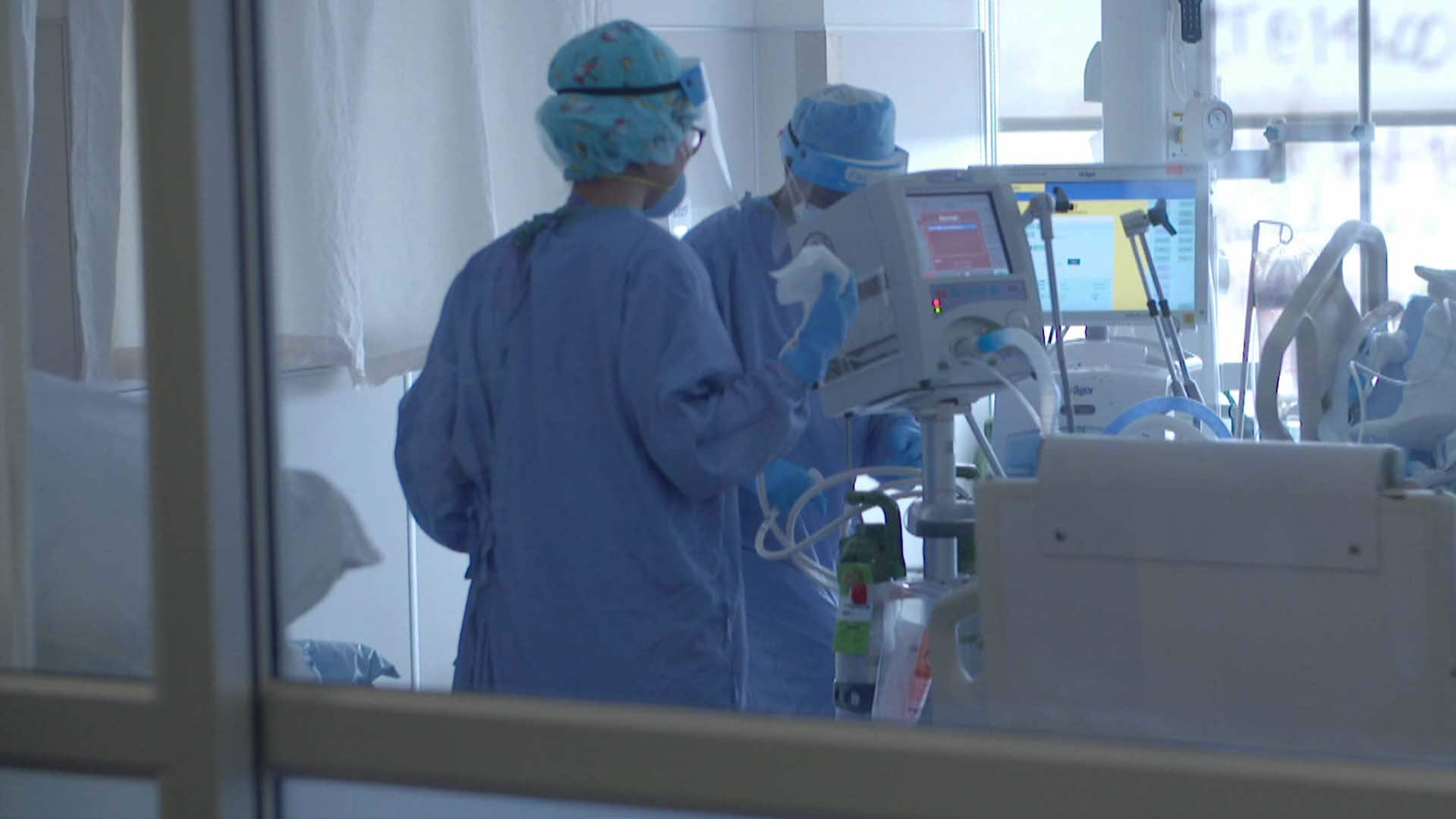
Even now, less than a month into the Omicron surge, more Ontarians and Quebecers are already in hospital with COVID-19 than at any other point in the pandemic, various provinces are cancelling scheduled surgeries for patients with cancer and other conditions and infections among health-care workers at multiple facilities are causing a crisis-level staffing crunch.
“I think in this wave we are going to see the consequences of a health-care system at its breaking point more than we will just see hospitals full of COVID patients,” Rasmussen said.
Possible ‘shift’ in pandemic
Many medical experts are urging people to avoid getting infected right now, if they can, while provincial leaders are bringing back such measures as virtual schooling, curfews and restrictions on indoor activities in hopes of slowing Omicron’s spread.
Yet stopping transmission of this variant is proving a daunting task — and plenty of Canadians can’t avoid exposure due to their jobs or living arrangements — so the harsh reality is that tens of thousands more people should expect to get COVID-19 in the weeks ahead, with some falling seriously ill while others experience lingering symptoms.
If this massive spike in infections does mark the coronavirus’s shift toward endemicity, Canada will have to decide what constitutes an acceptable level of COVID-19 infections, hospitalizations and deaths in the long term, said Dr. Srinivas Murthy, a clinical associate professor in the department of pediatrics at the University of British Columbia in Vancouver.
“Because it’s not going to be zero, and it’s not going to be our health system falling apart every single winter,” he said. “What it will be is somewhere in between, and it will mean hundreds of deaths per year or thousands of deaths per year, or what have you.”

There’s no guarantee Omicron will put Canada on that path, and inequity in global vaccination rates means much of the world remains largely unprotected against this virus — providing an ample supply of hosts to infect and opportunities for SARS-CoV-2 to continually evolve.
“Maybe we will get blanket immunity against Omicron and prior variants, but we have to appreciate that, if there is still transmission, there is still the opportunity for other variants to emerge,” said Jason Kindrachuk, an assistant professor in medical microbiology and infectious diseases at the University of Manitoba in Winnipeg.
“So I think that this could be a shift, certainly, in the pandemic … whether or not this is going to be the thing that changes overall patterns of transmission, I don’t know. And that’s something that I’m certainly concerned about.”
Living with virus may require ‘massive changes’
If the pandemic does begin to slide into an endemic state in Canada, we still don’t know what, exactly, that will look like and how often COVID-19 will flare up and disrupt day-to-day life.
Living with this virus long term, then, may require a complete rethink of our approach to keeping it at bay.
According to Yonatan Grad, the Melvin J. and Geraldine L. Glimcher Associate Professor of Immunology and Infectious Diseases at the Harvard T.H. Chan School of Public Health in Boston, that means making widespread investments in protection, such as masking and ventilation improvements.
“Past pandemics have led to massive changes in the way we live that we’ve come to accept as normal,” he said in a Q&A shared by Harvard in August.
“Screens on our doors and windows helped keep out mosquitos that carried yellow fever and malaria. Sewer systems and access to clean water helped eliminate typhoid and cholera epidemics. Perhaps the lessons learned from COVID-19 in terms of disease prevention can yield similar long-term improvements in individual and global health.”
But there’s no easy fix — and no way to predict exactly what the future will hold or how long any hard-won immunity from Omicron will last.
What’s clear is that COVID-19, in some form, is set to stick around — which means layering this illness on top of other viral infections such as influenza, which typically leads to an estimated 12,200 country-wide hospitalizations and 3,500 deaths each year.
Kindrachuk puts it this way: “How ready are we going to be to just add on another infectious disease to that potential list of things that we face, year after year after year?”













Leave a comment