Every Wednesday, a registered nurse travels 39 kilometres from the northeastern Alberta city of Cold Lake to see patients on the Elizabeth Métis Settlement.
Alberta Health Services rents an office inside the settlement’s community hall for appointments.
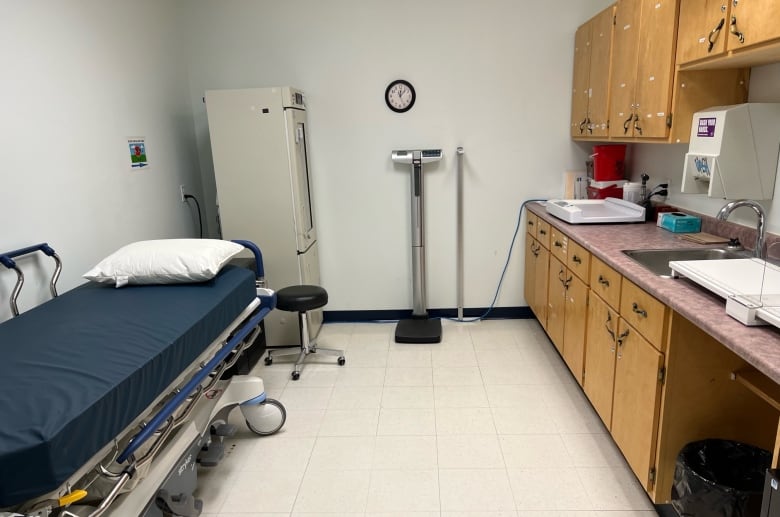
A counter near the door has a sink and a small weigh scale for babies, with a mobile hanging above it. On the other side of the room there’s a desk, a refrigerator for medicine and a bed for patients.
About three years ago the local registered nurse stopped working full-time in the community when she was hired for another position in Cold Lake.
“Nobody has filled that spot,” said Kathy Lepine, chair of the Elizabeth Métis Settlement council. “We kept posting it and posting it.”
Alberta Health Services says it is still recruiting a full-time registered nurse to serve the community of 640 people but hasn’t found one yet. The nurse who previously worked at the settlement full-time now works there once a week. Another nurse covers weekly home-care visits in the community.
The challenges facing Lepine and the Elizabeth Métis Settlement are not unique in Alberta. Many smaller communities are struggling to find adequate health care, due primarily to shortages of available doctors, nurses and other health-care providers.
Northern Alberta is home to eight self-governing Métis settlements with a combined population of 5,600 people; they are the only Métis communities in Canada with land-base agreements.
Canada has a patchwork system for delivering Indigenous health-care. Unlike many First Nations communities, where Indigenous Services Canada can provide federal funding to support health-care programs, health care for residents of Alberta’s Métis settlements falls exclusively under provincial jurisdiction.
“Métis settlements are Indigenous communities: living, breathing communities with infrastructure, health needs, water, youth programming, senior services,” said Lee Thom, a councillor for Kikino Métis Settlement, 185 km northeast of Edmonton.
“We’re stuck in a place where we’re not a municipality, but we’re not yet considered an Indigenous — for lack of a better word — federal community,” Thom said.

“So we’ve always been advocating for better services and there’s been some good steps made with the province now.”
For the first time in decades, there are now plans to have a doctor visit the Kikino Métis Settlement and two other settlements with a mobile clinic.
The move is among several recent commitments by the province to increase health-care resources within settlements.
But in the face of health-care staffing shortages, it may prove challenging to find the staff, said Canadian Medical Association president Dr. Alika Lafontaine, an anesthesiologist in Grande Prairie, Alta.
“It hasn’t been until recently that infrastructure has started to move into [Métis] settlements,” Lafontaine told CBC News.
“We’re now in a resource crunch across the country, so places that are traditionally under-resourced are now suffering even more in the broader context of the health system not having enough people to provide what’s needed.”
Mobile clinic in the works
Alberta Health Services has committed to providing a mobile clinic to travel between Kikino Métis Settlement and the neighbouring Buffalo Lake settlement. The same clinic may also visit Elizabeth Métis Settlement.
The clinic would use a vehicle provided by Telus through a health grant. Lepine, the Elizabeth Métis Settlement council chair, said she is hoping to see it visiting the communities by the fall.
Settlement leaders say a primary care provider for the mobile clinic — a physician or nurse practitioner — hasn’t been hired yet. A spokesperson for AHS said planning is ongoing.
A doctor can make a huge difference in the lives of people who live in settlements, according to Dean Ducharme, vice-chair of the Paddle Prairie Métis Settlement council.
Paddle Prairie has enjoyed better access to health care than other settlements, Ducharme said in an interview.
“Compared to the other seven settlements, it’s night and day,” he said.

The settlement built a space to house an AHS health unit that has two full-time nurses and a weekly prescriptions delivery service. For nearly a decade, Paddle Prairie has had a doctor visit once a week.
“It’s been nothing but a success story,” Ducharme said. “Every time he comes, he’s booked right from 9 to 4:30; he’s got client after client after client.”
Ducharme said the health centre is essential for many residents who don’t have transportation to travel the 70 kilometres to the nearest hospital in High Level, which has long wait times and serves eight First Nations communities.
Health board pushes for change
New projects underway have come about after 10 years of work by Métis settlements to advocate for better resources and implement new programs in their communities. In 2013, the eight settlements formed a health board to lobby AHS for better services.
Ducharme said bringing the mobile clinic to more settlements is the biggest goal for the health board, and he’s optimistic that new funding announced will help make a difference.
Lepine, who is also the chair of the Métis Settlements Health Board, said she has seen improvement in the last year since Health Minister Jason Copping began meeting with settlement representatives.
In February, the East Prairie Métis Settlement near High Prairie received $20,000 for a virtual care clinic that will allow settlement members to see a doctor through online appointments. The same month, AHS received $300,000 to train two medical first responders in each Métis settlement. AHS said the program is set to roll out later this year.
Fishing Lake Métis Settlement, a community of 600 people 70 km northeast of Elk Point, is expecting a doctor to begin travelling to the community this spring, said Coun. Arlene Calliou, who sits on the health board.
In an e-mail, AHS confirmed it will provide a physician to travel to the community, but couldn’t provide a start date.
It’s not clear when all the health-care positions promised to Métis settlements will be filled, given the shortage of physicians and nurses. Different levels of government in Canada have historically neglected to provide adequate health care for Indigenous communities.
“Indigenous patients — First Nations and Métis mainly in Alberta — have to travel away from their home communities in order to receive care,” said Lafontaine, the CMA president, who previously led the Indigenous Health Alliance project.
“A forest camp is required to have a strategy to insure 24/7 availability of a doctor or primary care assessment,” he said.
“But we have areas of the provinces, and areas across the country — including Métis settlements and First Nations across Canada — where you don’t actually have a primary care provider for large parts of the month.”
Racism creates more obstacles
Lepine, chair of the Métis Settlements Health Board, said an additional barrier to care is that some people have had negative experiences with health-care workers outside their communities.
CBC News interviewed several settlement members who expressed reluctance to seek medical attention at some hospitals for fear of being neglected or mistreated. Settlement leaders also expressed concerns about stereotyping and racism leading to a poorer quality of care.
“The challenge is the treatment that you get when you go to emergency doctors,” Lepine said. “It’s real and it’s there.”
Shawn Daniels, who lives in Elizabeth Métis Settlement, said that in 2021, he cut his hand on a glass while washing dishes. He went to a hospital’s emergency department to get stitches but said that after hours of waiting, a doctor turned him away, telling him it was too late to deal with the injury. He hadn’t been offered Tylenol or a bandage, he said.

Daniels went to a different hospital the next day, where a doctor saw that he was still bleeding and gave him stitches. He later lodged a complaint with AHS about the treatment he received at the first hospital.
“Honestly, I think it’s because I’m the wrong colour,” Daniels said. “Something doesn’t seem to add up when you’re the first one there and the last one to be seen.”
Doug Bellerose, a councillor with East Prairie Métis Settlement, also said addressing racist stereotypes is one of his major health-care concerns. Bellerose recalled a hospital trip when his teenage son had food poisoning at an out-of-town hockey tournament.
“The first question they asked him was ‘Are you doing coke? Are you on drugs?'” Bellerose said.
Daniels said he would like to see more anti-bias training for medical students.
In 2022, the AHS north zone created a dedicated support line for Indigenous peoples to help them navigate the health system. It is staffed by Indigenous Health Link staff.












































Leave a comment