As demand drastically increases for COVID-19 testing across the country, experts say it will quickly become harder to get an exact picture of Omicron case counts in Canada.
And that means health authorities are likely soon going to have to rely more on hospitalization numbers as the main indicator of the extent of the impact of the new coronavirus variant.
“This is such a hyper-contagious disease that it was completely foreseeable … that the rate of spread would overwhelm the testing capacity that we have, as is already happening,” said Raywat Deonandan, an epidemiologist and associate professor at the University of Ottawa.
COVID-19 case counts have never been perfect, but now with Omicron’s highly contagious nature, polymerase chain reaction (PCR) testing has been maxed out in some provinces as people rush to get tested.
With some areas expected to limit who can get tested, health experts say that will lead to an undercount in cases.

Others say case counts become less important if symptoms are milder, and that tracking hospitalizations, death counts and the strain on the already maxed-out health-care system is more important at this time.
“At the end of the day, we’re trying to prevent people from getting severely ill and people from dying. So those hospitalization rates are important,” said Dr. Stephanie Smith, an infectious disease specialist at Edmonton’s University of Alberta.
“Many hospitals are just trying to recover from the last wave, the Delta wave, and really have not fully recovered. So even a small increase in hospitalizations due to Omicron is challenging.”
WATCH | Why experts say COVID-19 numbers are much higher than recorded:
Epidemiologists Dr. Peter Jüni and the U.K.’s John Edmunds say the number of COVID-19 cases is vastly undercounted. They also say global co-operation among experts is helping inform them faster about the rapidly evolving coronavirus. (Francis Ferland/CBC) 6:23
PCR testing systems struggling
While most provinces have made rapid tests more widely available, PCR tests are still considered the gold standard of COVID-19 testing, with the main advantage being that the tests are much more sensitive and highly accurate.
But with PCR test sites clogging up in some provinces due to high demand right before the holidays, case counts aren’t being fully captured.
That’s what’s happening in Ontario, according to one doctor.
“Typically in Ontario, if things are quite OK and the surveillance works, we assume that we detect roughly 40 per cent of the cases. But what we see now is that the surveillance system starts to struggle,” said Dr. Peter Jüni, the scientific director of Ontario’s Science Advisory Table.
He estimates Ontario is now detecting about 30 per cent of the COVID-19 cases. That means if there are 3,000 confirmed cases, the actual number could be closer to 10,000 cases.
“These numbers will be an undercount, and will become more and more unreliable as case numbers are growing,” he said.
Just part of the long line of drivers waiting for a Covid test in Vancouver right now. <a href=”https://twitter.com/hashtag/covid?src=hash&ref_src=twsrc%5Etfw”>#covid</a>-19 <a href=”https://t.co/9NTuVugldA”>pic.twitter.com/9NTuVugldA</a>
—@ianhanomansing
Just how fast Omicron can spread is still being reviewed by researchers around the world.
A research team in Hong Kong recently found the variant may be multiplying 70 times quicker than earlier strains within our lower airways, though the lab-based study is still undergoing peer review ahead of publication.
Numbers suggest Omicron has a doubling time of two to three days, giving it what the World Health Organization has called a “substantial growth advantage” over Delta.
Because of that rapid spread, Deonandan expects PCR testing systems to max out in many provinces. He also expects there to soon be limits on who can get tested on the provincial level.
“It seems likely that everybody’s going to get exposed sooner rather than later — talking weeks, not years,” he said.
“And as a result, we’ve never had the testing capacity to test everybody in the country in a short period of time.”
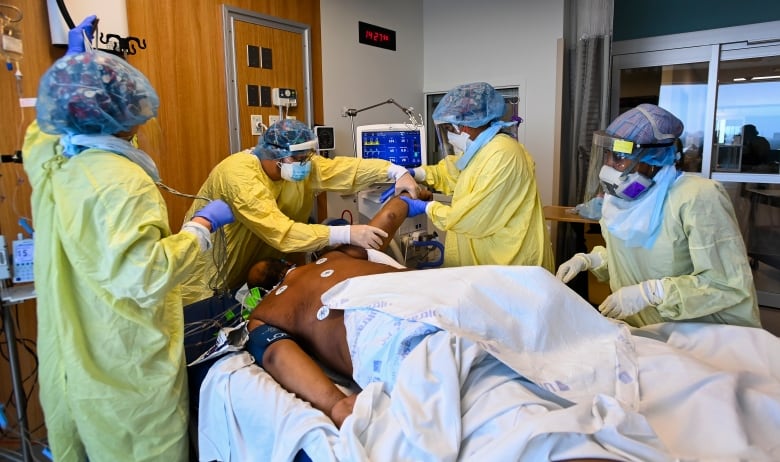
While tracking community spread through testing is initially important to try to figure out just how rapidly the virus is spreading, said Smith, looking at hospitalizations is “more robust and an important metric in terms of looking at the impact on the health-care system and on society.”
However, hospitalizations are a lagging indicator, she said, and it could take a few weeks before we see the results of high community transmission on hospitalization numbers.
On Tuesday, Ontario’s Chief Medical Officer of Health Dr. Kieran Moore said the province’s health authorities now have “laser vision” on hospitalization rates.
“That is trending up,” he said.

The threat to hospitals continues to come from those who have never been vaccinated or infected with COVID-19, said Jüni.
“These people before actually derived a lot of protection by vaccinated people. But what we see now is protection against infection melts like snow in the sun with Omicron if we only have had two doses,” he said.
“It’s extremely important just to make it to the three doses, to gain time with public health measures now and make sure that we now start to slow this explosive growth here.”
Milder symptoms
Some of the earliest data from around the world suggests that many people infected with the Omicron variant ended up with milder symptoms.
Most of the cases in the European Union have also been mild or asymptomatic, according to a report Monday from the European Centre for Disease Prevention and Control. A preliminary analysis from South Africa also said Omicron appears to be milder.
But there are three key caveats to that early data.
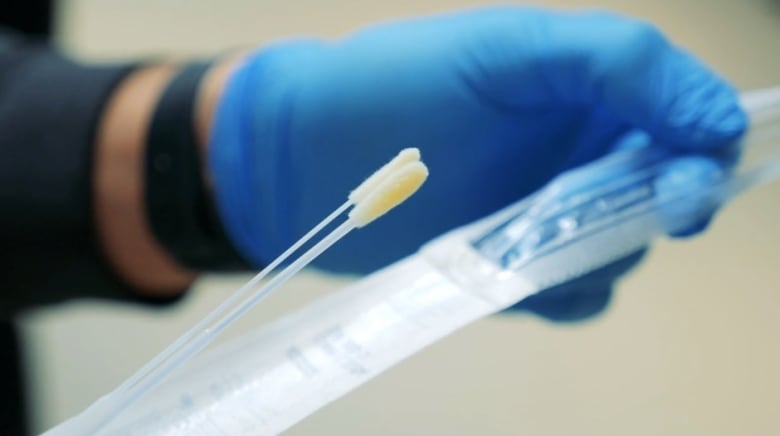
First, Omicron might seem mild because it’s largely hitting younger people — the same age group already less likely to be hospitalized or end up with severe disease from COVID-19.
Second, more people are likely to have some level of immunity at this stage of the pandemic, either through vaccination or a previous COVID-19 infection.
Third, there haven’t been enough cases to properly represent entire populations. The European agency cautioned it would need hundreds more cases to accurately assess how Omicron differs from previously detected variants.
In Denmark, for example, despite the fact that they’re recording 7,000 to 10,000 cases per day, hospitalization rates are just starting to increase, said Dr. Dan Gregson, an infectious disease specialist and associate professor in the Cumming School of Medicine at the University of Calgary.
“It’s been a relatively slow climb, rather than this big, straight wall that we’ve seen with cases,” he said. “We’ll keep our fingers crossed for that.”
In order to protect Canada’s hospitals, Canada’s Chief Public Health Officer Dr. Theresa Tam told The National this week that now is not the time to be gathering in big numbers.
“Even if Omicron happens to be milder than the previous virus variants, because it’s spreading so rapidly … even a small proportion of people winding up in hospital is going to overwhelm our systems,” she said.
WATCH | Top doctor calls for Canadians to reduce contacts over the holidays:
Dr. Theresa Tam, Canada’s chief public health officer, says the only way to prevent huge numbers of patients from winding up in hospital with COVID-19 in the coming weeks is to reduce gatherings over the holidays. (Evan Mitsui/CBC) 1:08
Meanwhile, Deonandan says greater reliance on data derived from at-home rapid tests could help officials shed more light on community spread, particularly if it could be incorporated into COVID-19 modelling.
Positive symptomatic screening could also be useful, he said. The epidemiologist pointed to the AIDS crisis, when the Bangui definition was created, relying on a checklist of symptoms to diagnose when HIV testing wasn’t available.
A similar approach to COVID-19 symptoms and exposure risk could be applied, said Deonandan.
“It will be useful to collect information on the people who satisfy those criteria. So not just positive PCR tests, but positive symptomatic screening.”
Ultimately people shouldn’t panic, Deonandan said, but rather show concern about the potential effects of Omicron on the health-care system and the general population.
“The reason we self-restrict, impose all these restrictions, is to preserve this system. So don’t panic. Recognize this is about keeping society afloat.”












































Leave a comment