Doctors in Alberta say a countrywide shortage of anesthesiologists is taking a toll on surgery patients in the province.
According to the Canadian Anesthesiologists’ Society, Canada has far fewer anesthesiologists for every 100,000 people than other countries, including the United States and Australia.
The organization says that is contributing to surgical delays around the country.
In the central Alberta city of Red Deer, doctors say operating rooms are now regularly shuttered because there aren’t any anesthesiologists available.
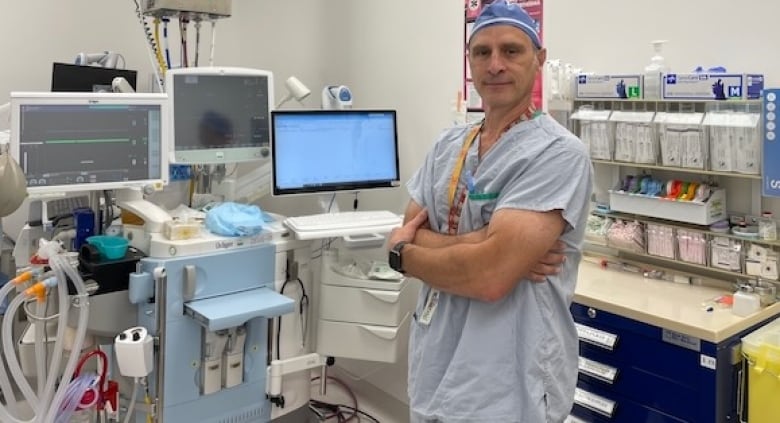
“Our situation is quite dire,” said Dr. Trevor Rudge, who is one of the few left.
“We need 50 per cent more anesthesiologists. We have about half the number we need.”
According to Rudge, that means elective surgeries ranging from hysterectomies to hip and knee replacements are being cancelled.
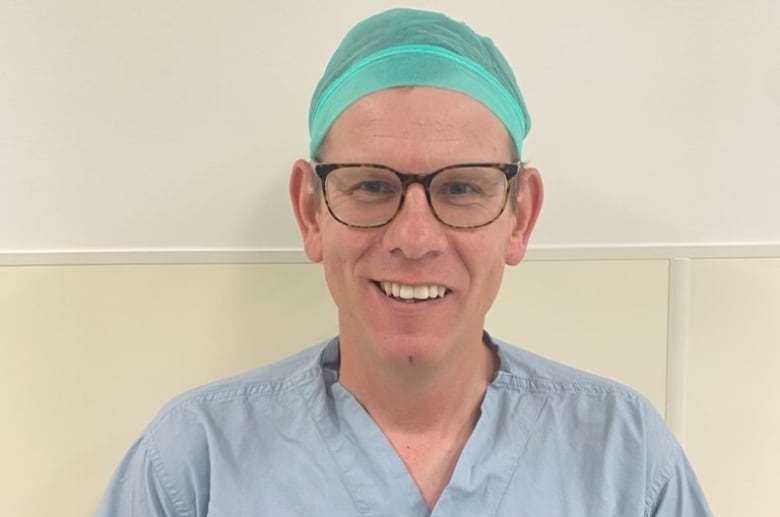
It’s a big concern for Dr. Keith Wolstenholme, a Red Deer orthopedic surgeon, who is watching his wait-list grow.
“What it means is less patients getting their surgery in a timely manner,” he said.
“Come September, it’s two years since we’ve run full capacity. It’s honestly getting a little bit hard to have hope.”
Large urban centres also affected, doctors say
Red Deer was hit early — and hard — by the shortage. But larger cities are feeling the pinch now, too, according to doctors.
Dr. Kevin Gregg, an Edmonton anesthesiologist, said COVID-related burnout, an aging workforce and a rocky relationship with the Alberta government are driving physicians away.
“Those people aren’t being replaced. I’ve heard relatively scary numbers about what we’re looking at in the fall,” said Gregg, who is also the section president for anesthesia with the Alberta Medical Association.
He worries operating room closures could start happening in Edmonton in the coming months.
“You can’t create people. It’s stressful,” said Gregg. “I don’t think there’s a magic bullet.”

Calgary, while not as hard hit, is also seeing impacts, according to Dr. Craig Pearce, an anesthesiologist at the Peter Lougheed Centre.
“The anesthesia shortage is pervasive. It’s all across Canada. It’s all across North America,” said Pearce.
“We have huge wait-lists and we have empty operating rooms and operating facilities that we could use that we can’t.”
Recruitment underway, AHS says
Alberta Health Services did not answer questions about operating room closures but said it is working to recruit anesthesiologists around the province.
According to the health authority, 470 anesthesiologists were working for AHS as of July 13, an increase of 20 since the end of March.
In a statement, AHS said it’s recruiting for 65 positions, including both permanent and locum positions.
“Some of these positions have already been filled and others are in the offer stage,” spokesperson James Wood said in an email, adding 40 of those are new positions.
All this comes at a time when Alberta is trying to reduce its surgical backlog and boost the number of publicly funded procedures performed through contracted private surgical facilities.
AHS said it aims to conduct a total of 310,000 surgeries (in hospitals and chartered facilities) this fiscal year compared with 292,500 last year.
With the increased use of private facilities, Wolstenholme wants to see safeguards in place to protect the hospital system from losing anesthesiologists to these facilities.
“There needs to be some measure to make sure that … the hospital system is still served so that patients, when they come in at their sickest, still have qualified workers to look after them,” Wolstenholme said.
AHS said its anesthesiologists and surgeons are sent to private facilities only to do work under publicly funded contracts.
Canada-wide shortage
The Canadian Anesthesiologists’ Society has been trying to raise the alarm about the shortage for years.
“I am very concerned about the shortage of anesthesiologists in the country. Despite a near doubling of physician anesthesia providers in the past 20 years, today’s demand outstrips our current supply,” Dr. Lucie Filteau, the group’s president, said in an email.
“Operating room closures (and postponement of surgeries) are happening on a daily basis across the country due to human resource constraints.”
Filteau said shortages of other operating room staff and a lack of hospital beds also contribute to the problem.
One key step, according to the group, is the use of anesthesia care teams (ACTs), which have been implemented, to varying degrees, around the country.
Anesthesia care teams
In Alberta, ACTs allow one anesthesiologist to oversee more than one operating room at a time, with the support of respiratory therapists for some minor procedures.
A pilot project was launched by AHS last year using this system for cataract surgeries.
“AHS is expanding the anesthesia care team (ACT) model in cases where this model has been shown to be safe, effective and efficient,” said Wood, adding the model is now being used for podiatry surgeries in the Calgary zone.
Pearce cautions that expanding the use of ACTs must be done with safety in mind.
“The fact that we are now slowly being diverted and replaced along the way is just further evidence of how severe the situation is,” he said.
According to Pearce, there are also efforts to increase anesthesia training spots and to use more family physicians who are specially trained in anesthesia.











































Leave a comment