Nancy Mullin remembers the call last June. Staff at the Garden Home, a private long-term care facility in Charlottetown, had found a small wound on her mother Helena’s heel. She was heading to the Queen Elizabeth Hospital for treatment.
The family was optimistic that with proper care, the pressure wound, or bedsore, would get better.
But as the wound began to fester, so did Nancy Mullin’s distrust of the care her mother was receiving.
Helena was born in 1929, the youngest of 15 children. Growing up, Mullin remembers her mom with a “beautiful manicure” and a pound cake always on standby for anyone who needed a boost.

Her family had been mostly satisfied with the care Helena received for six years at the long-term care home.
But Mullin was beginning to worry that the staff were stretched too thin or insufficiently trained to properly care for her mother, who also had diabetes. Her sister put a sign-in sheet on the wall and asked staff to make sure they recorded each time they came in and provided care.
Still, over the course of three months, the wound grew.
“It was just getting bigger all the time,” said Mullin.

Garden Home has been operating on a provisional licence since January 2022. That means the Community Care Facility and Nursing Home Board, which oversees all private long-term care homes on P.E.I., determined it requires improvements to meet the inspection standards.
Over the last year, seven of the 10 private long-term care homes on the Island have failed to meet the inspection standards needed to receive a full licence at one time or another. Four of those are still listed as having a provisional licence: Clinton View Lodge, South Shore Villa, Whisperwood Villa and Garden Home.
CBC News has reviewed the inspection reports associated with the provisional licences and found facilities lacking in differing areas such as:
- Incident reporting and risk management practices.
- Safety checks and risk assessments.
- Pressure sore assessment and interventions.
- Having a registered nurse as the designated director of nursing or director of resident care.
- Orientation training for new staff.
More licensing adjustments could be coming.
According to the province, licensing letters were sent to Clinton View Lodge, South Shore Villa and Garden Home Villa on Jan. 25. If the homes do not file an appeal within 10 days, the updated decisions will be posted publicly on Feb. 9. This means the homes could see provisional licensing extended or lifted, or additional measures could be imposed, such as a freeze on new admissions.
The province would not comment on what changes are coming for the homes before the appeal period is over. It is possible one or more have recently met requirements.
Shut down not likely
“These aren’t just letters going out … people are living right now in what’s going on there,” said Louise Hall, president of Save our Seniors Canada, a group advocating for those in long-term care.
“It seems things are getting worse instead of better — and the stories, the stories that are coming out, they’re heartbreaking.”
If you have information about this story, or a story to share with CBC Prince Edward Island, please email sheehan.desjardins@cbc.ca
But in the face of the province’s long wait-list for long-term care beds, a shut down is a last resort, according to the Community Care Facility and Nursing Home Board.
“The reality is that the closure of any long-term care facility would have significant negative impacts on the province as a whole,” the board told CBC News in an email in December.
“There are already insufficient spaces for all P.E.I. residents who want or require admission to a community care or nursing home facility and closure of any facility would place an increasing pressure on facilities that remain open and hospitals who may be required to provide continuing care when no facilities are available.”
According to Health P.E.I., about 165 people are already waiting for a long-term care bed; 42 of those are waiting in hospital.
‘We’re in crisis mode’
In P.E.I., private homes receive yearly scheduled inspections evaluating areas such as staffing, medication management and infection control. The home then receives a rating of compliant, partially compliant or non-compliant.
The board says there is no specific score or measurement that differentiates between partially compliant and non-compliant facilities. Nor is there a maximum number of provisional licences one home can get before being shut down.
But some operators say they can’t meet requirements because they are understaffed and don’t have the money to fix the problem.
“It’s a disaster,” said Ramsay Duff, president of the Nursing Home Association of P.E.I. and CEO of the MacLeod Group of seniors homes, in November.
“It’s not a question of being fragile. We’re in crisis mode.”
Private, provisionally licensed care
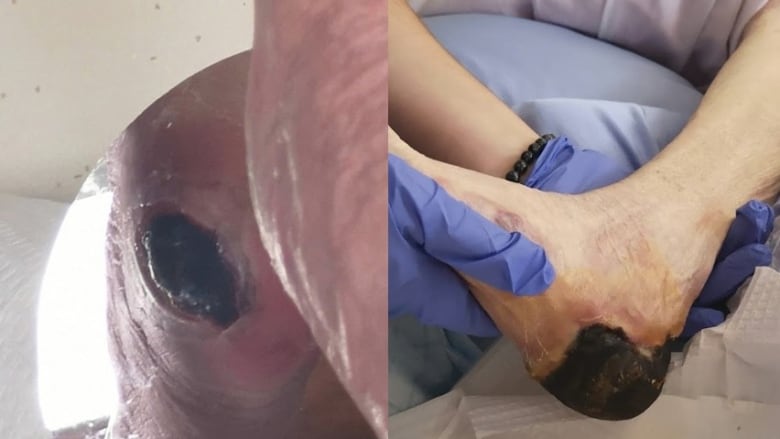
Crisis mode is exactly what the family of Helena Mullin felt they were in. They decided to move their mother to another home when the wound that had started out the size of a loonie grew to black, necrotic flesh creeping up the back of her heel.
Nancy Mullin said her family was displeased with how they sometimes found Helena’s pressure boot with pus inside and a foul smell emanating from it.
They moved their mother to Beach Grove Home, a public long-term care facility. They say they felt better about her care there, citing things like better communication, a better bed, wheelchair and more attention to even non-essential details, such as keeping her mother’s belongings in order, and doing her hair and nails.
Though they were happy with the move, the wound did not begin to heal.
Helena Mullin died on Oct. 5, 2022. Her medical record from the home notes she was suffering from “sepsis do [sic] to chronic wound.”

There is no documented evidence to suggest that this wound should have healed, but Nancy Mullin said they can’t help but feel the outcome would have been different if their mom had received different care.
“Pressure injuries on the heel area is probably one of the most difficult areas to manage once the injury has occurred,” said Kevin Woo, a professor at Queen’s University and the president of the Canadian Pressure Injury Advisory Council.
“Having said that, it doesn’t mean that it’s not possible. I think we just have to look at the kind of care that is required.”
Complaint reviewed
The family did file a complaint with the Department of Health and Wellness. In an email to the family, the department confirmed the complaint had been reviewed with the facility.
“Based on your concerns you presented at that time, the care service and dietary inspectors were both involved in reviewing your complaint. The outcome indicated there was additional work the home had to do on the identified standard ‘4.4.13 – A resident with potential for altered skin integrity has a plan in place to prevent deterioration and to ensure appropriate skin care and wound management is conducted as required. This includes promoting healing, optimizing nutritional intake, preventing infection and minimizing pain and discomfort.'”
The province told CBC News it would not comment on an individual patient’s case.
CBC News requested an interview in December with the CEO of P.E.I. Seniors Homes, the group that operates the Garden Home and Whisperwood Villa, but was told he is “not able to comment publicly on specific family members’ concerns.” CBC News reached out for comment again in January but did not receive a reply.
Seeking change
Looking back, the Mullin family is devastated, saying something needs to change in the way private long-term care is provided on P.E.I.
“This cannot happen to anybody else’s loved one,” said Mullin. “These people paid their taxes, they did their dues, they raised children. You know, they didn’t do anything wrong. Why are they being treated like this? It’s awful.”
The program director for the wound care institute at York University said more education around wound care is needed across the country.
“I think everybody tries to do the right thing but the issue to me is limited knowledge,” said Rosemary Kohr. “It’s really important to pay attention because the outcome can be sepsis and can lead to amputation or death.”
Beds sitting empty
While the province says it can’t afford to close entire homes, it is closing beds to try and regulate more time spent with fewer residents in private homes.
MacLeod Group operates Clinton View Lodge and South Shore Villa. South Shore Villa had been operating under an admission freeze that was lifted in November. Clinton View Lodge was also operating under an admission freeze that was set to be re-evaluated on Jan. 18. The province said a decision has been sent to the facility, which will be made public following the appeal period.
As Islanders continue to sit on the wait-list, more than 50 long-term care beds across the province are also sitting empty because facilities don’t have enough staff.
The Nursing Home Association says residents are “receiving the quality care that’s required under the Act,” but they need staff.
“We’ve been experiencing labour shortages because staff are leaving mainly for higher wages in the public manor system,” Duff said.

At the time of a 2021 Long-Term Care Review put forward by the P.E.I. Department of Health and Wellness, public care workers made $21 to $22 per hour, while private care workers were paid between $12 and $19 per hour. Minimum wage has since increased to $14.50.
“Until we can get back up to our regular staffing levels, those beds are going to remain closed,” Duff said.
The MacLeod Group alone had around 30 job vacancies in November. Duff said some homes are now turning to “agency staff” — staff hired on temporary contracts through private companies — to fill in the gaps. He said the staff are qualified to work but sometimes don’t get the orientation required by the licensing board.
“That’s been difficult to do because we want them on the floor working so we can have those beds open,” he said.
“This comes back to government funding, and right now, we essentially have two-tier funding in our province…. I think we’re in a crisis and the government is just ignoring it.”
Contract frozen
The funding agreement between private long-term care operators and the P.E.I. government expired in 2020. That means the operators are still locked in at that rate despite the current costs to operate.
In Nova Scotia, for example, Duff said the government gives the average private long-term care home approximately $240 per patient per day. On P.E.I., he said private homes receive about $135 while public manors get closer to $280.
However, the province added it’s important to note the services are not exactly the same. Private homes tend to have more personal care workers, rather than a complement that includes more RNs and LPNs in the public care model, which costs more.
“Until government fixes that funding piece that allows us to then start hiring, secure our workforce, be able to recruit properly, staff every shift, not have agency staff in place, this is just going to continue to be a problem for us,” said Duff.
The P.E.I. Department of Health and Wellness declined to comment on negotiations and said in an email they are “in active talks” with long-term care operators.













Leave a comment