In the 1990s, after enduring the uncertainty of seasonal work, Kanaiya Gandhi was offered a job at a Toronto-area factory.
It was an ideal move for the young married man who had immigrated to Canada from India just a decade before: regular hours, stable work and the security of a union. As the years passed, Gandhi became an experienced machine operator, building acoustic panels for various airports and arenas while providing for his wife and two daughters in Brampton, Ont.
But one of his daughters, Radhika, said the factory was also the place where her father caught COVID-19.
After he fell ill in December 2020, Radhika kept in touch with Gandhi’s manager at the factory, who told her more and more workers were getting sick — all while her dad’s own situation was deteriorating at home, prompting her to call 911 in early January 2021, after he began struggling to breathe.
About a month later, Gandhi passed away in hospital at the age of 58. He’d spent 26 years of his life working on the factory line.
Looking back on her family’s loss, Radhika said being an essential worker put her father at a higher risk of contracting the virus, along with so many other Canadians from largely racialized, lower-income neighborhoods.
“Anyone could tell you that people of colour and marginalized communities face a lot of health inequities,” she said.
There’s now new data backing that up, thanks to findings from a Canadian research team that suggest COVID-19 disproportionately impacted certain communities throughout much of the pandemic.
Cases ‘disproportionately concentrated’
Published on Monday in the Canadian Medical Association Journal (CMAJ), the new peer-reviewed study analyzed COVID-19 cases in various regions between January 2020 and the end of February 2021 to understand which areas were hardest hit.
The team linked COVID-19 surveillance data with demographic breakdowns from 16 Census Metropolitan Areas (CMAs) — which can include major cities and surrounding regions — in British Columbia, Manitoba, Ontario and Quebec, the four provinces that accounted for the bulk of Canada’s cases in the pandemic’s first year. (Long-term care cases were excluded, to instead focus on transmission in the community.)
The researchers found that cases were “disproportionately concentrated” in areas with lower incomes and education levels, along with a higher proportion of visible minorities, recent immigrants, high-density housing and essential workers.
“We kind of expected from what we saw on the ground and from reports from local public health units that we would see this pattern,” said lead author Mathieu Maheu-Giroux, an assistant professor in McGill University’s department of epidemiology, biostatistics and occupational health in Montreal.
“But it was quite striking to see this consistency.”

In the Toronto CMA, for instance — which includes surrounding areas such as Brampton, where the Gandhi family lived — 50 per cent of the reported COVID-19 cases during the study period were clustered in areas with roughly 30 per cent of the population.
There was a similar breakdown in Montreal, while in the Vancouver area, 50 per cent of the cases were borne by communities with just a quarter of the population.
“It’s nice to have national representative data saying this is what’s going on in all of our major cities,” said Dr. Srinivas Murthy, a clinical associate professor at the University of British Columbia in Vancouver and a research chair in pandemic preparedness. He said this was a straightforward study despite the limited demographic data available, including a lack of current census information and gaps in the data on individual cases.
Explosive transmission at factories, warehouses
Throughout the pandemic, various studies have uncovered similar disparities, while health-care workers and community groups have long highlighted the inequalities underpinning these infection trends.
While much of the country shifted to remote work early on — particularly during periods of lockdowns or heightened restrictions — essential workers kept heading to their jobs, hiking their risk of catching the virus.
There were examples of explosive transmission at workplaces across the country — from more than 600 COVID-19 cases tied to a months-long outbreak at an Amazon warehouse facility outside Toronto, to a staggering 950-worker outbreak at an Alberta slaughterhouse in 2020 that was linked to three deaths, including one employee’s elderly father.

Advocates also raised concerns over high rates of household transmission experienced by multigenerational and immigrant families, often living in crowded housing.
And back in March 2021, data released by Statistics Canada showed that the country’s most racially diverse neighbourhoods had COVID-19 mortality rates more than twice as high as those reported by districts that are overwhelmingly white.
Several front-line workers and medical experts who spoke to CBC News said the new CMAJ study echoes locally reported data and those early alarm bells.
“COVID-19 does not impact us all equally. People who are living in situations where they’re considered to be structurally vulnerable are more likely to get hit by the virus,” said Dr. Naheed Dosani, the health equity lead for Kensington Health, a community care organization in Toronto.
“I hope that this research — and all the discussions we’ve had in this pandemic about health inequities — will educate us and put us in a position where we react to future scenarios like a pandemic knowing some people are more at risk than others.”
Dosani stressed the need for supports tailored to certain communities, such as vaccination pop-up clinics and resources in viral hot spots.

In the Toronto area, there have been after-hours vaccination clinics for shift workers, teams bringing vaccines directly into highrise buildings where seniors live and local organizations translating educational materials into a variety of languages.
In Montreal, meanwhile, outreach workers going door-to-door sharing vaccination information over the last year realized that in neighbourhoods with more new immigrants and low-income families, it was more effective to stop by at night, since people were typically out working during the day.
Hard-hit neighbourhoods also need more investment and resources, including broad access to testing, said Vhil Castillejos, the manager of community well-being at the Jane/Finch Community and Family Centre in Toronto’s northwest.
“I just hope that this study can support some of the demands and claims the community has been asking for such a long time and actually get it through to decision-makers,” he said.
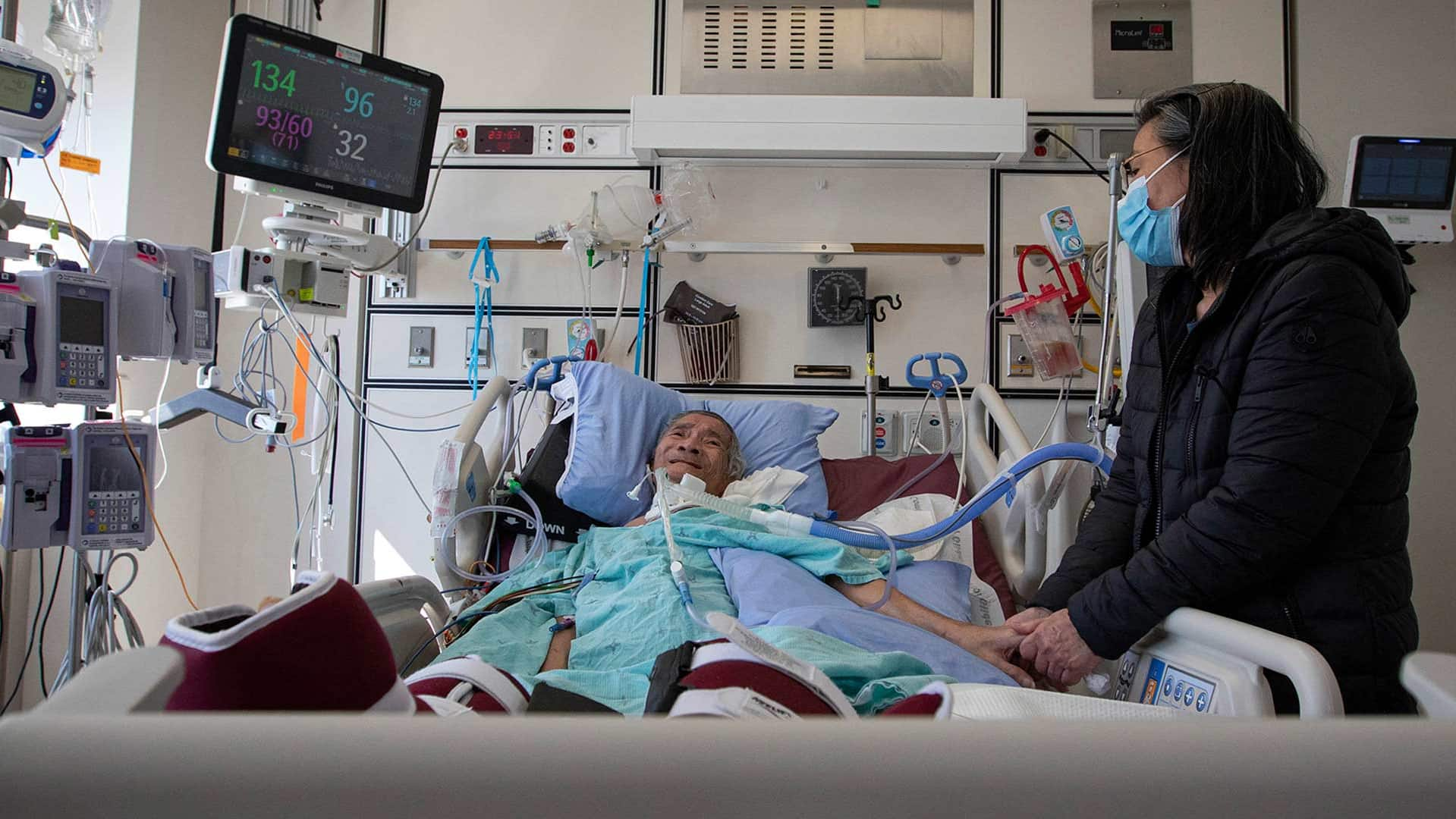
More patients are fighting for their lives in Ontario ICUs than at any previous point in the pandemic. CBC News goes inside Toronto’s Scarborough Health Network to see the impact. 6:36
Study period didn’t cover variants like Omicron
The CMAJ study’s research period, covering just the first year of the pandemic, didn’t capture all of the shifts in severity and transmission tied to various variants that emerged throughout 2021.
The Omicron variant, most recently, led to unprecedented case counts across the country — hitting millions of Canadians who had managed to avoid infection for two years.
With access to PCR or rapid tests now limited in much of Canada, lead study author Maheu-Giroux said it would be difficult to conduct a similar analysis to know which communities have been most impacted by the Omicron wave. But he suspects there would be similar findings.

“Omicron is more transmissible, more people are acquiring it, but it should still spread faster in high-density housing and census areas where there are more essential workers because these individuals have more contacts,” he said. “What might change is the level of prior immunity.”
Radhika Gandhi, whose father died from COVID-19, says she’s worried her family’s experience may be repeated for others as provinces continue lifting restrictions.
“I fear that COVID cases are going to skyrocket again, and again, you’re going to have marginalized communities facing the worst of it,” she said.
Now an epidemiologist in training, Radhika says she hopes to continue unpacking disparities in health care, fuelled in part by witnessing her father’s battle with COVID-19. And she says it’s crucial that governments understand which communities are most at risk during pandemics like this one, since “policies need to be guided by science when it comes to protecting community members.”
Targeted outreach, sick days, health-care benefits and a living wage are all ways to better support vulnerable essential workers during this pandemic and beyond, Radhika said.
“There are so many different social determinants at play,” she added. “It’s hard addressing them, but that doesn’t mean we shouldn’t take a step forward.”











































Leave a comment