Intensive care physicians and nurses share their concerns as they brace for an influx of patients that threatens to overwhelm hospitals due to the resurgence of the coronavirus and the flu.
When Canadians successfully flattened epidemic curves during the summer, the goal was to prevent hospitals and intensive care units from facing a crush of too many patients with COVID-19 all at once. Health officials wanted to avoid what happened in hospitals in New York City, where refrigerated trailers were used as temporary morgues.
But the recent surge of new coronavirus cases in all provinces beyond Atlantic Canada has already thwarted surgery plans and led to the cancellation of surgeries such as hip replacements at one hospital in Toronto and postponements in Edmonton.
Dr. Bram Rochwerg, an associate professor at McMaster University and critical care lead at the Juravinski Hospital in Hamilton, anticipates a surge of patients with COVID-19, and he worries they won’t be able to accommodate them all as more surgeries resume.
Unlike in the spring, beds and crucial staffing need to be reserved for medical and surgery patients, too. Traditionally, autumn in hospitals means scrambling for health-care workers such as nurses and respiratory therapists to backfill those sick with the cold and flu or who need to stay home to care for sick children.
“We’re all worried about it,” Rochwerg said. “You see the provincial [COVID-19] numbers creep up day by day. We see that critical care numbers [of ICU patients] creep up.”

The challenge, Rochwerg said, is to find a balance between adding restrictions to protect vulnerable populations such as residents in long-term care homes while preserving crucial aspects of society.
Lessons learned
Rochwerg also pointed to several lessons physicians worldwide have learned to help take better care of patients critically ill with COVID-19 during the resurgence.
“We should treat them like we would any other patient,” he said. “Sometimes, you just need [to insert] a breathing tube.”
When patients are on a ventilator, it takes the skilled hands of four to six hospital staff, including a respiratory therapist who regularly checks the breathing set up and tubing to ensure the airway is protected, as well as nurses to safely turn or “prone” them onto the stomach to improve ventilation.
WATCH | COVID-19 resurgence raises hospital capacity concerns:
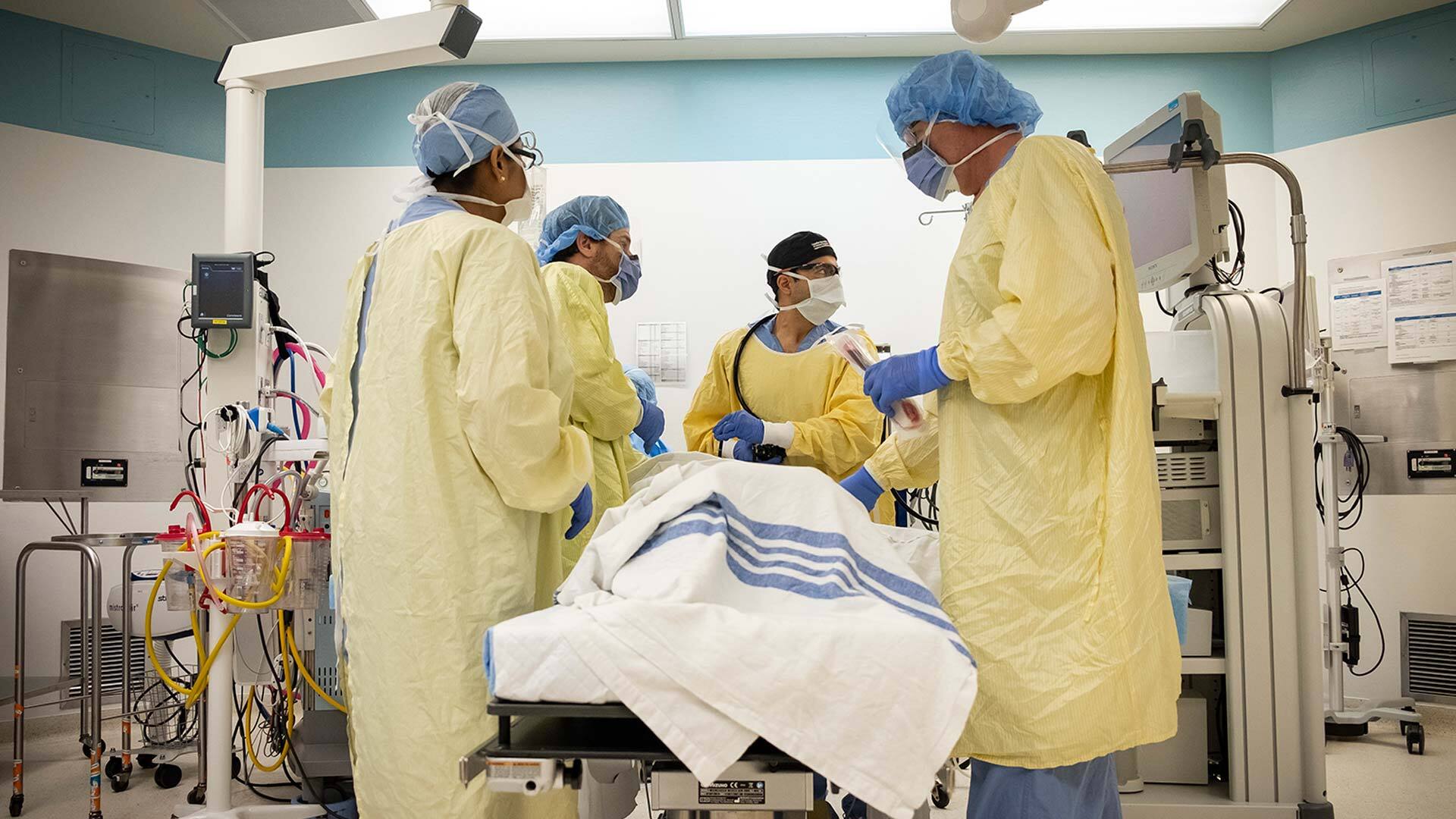
There is growing concern that Ontario hospitals and ICUs, especially in Ottawa and Toronto, may not have enough capacity for COVID-19 patients after weeks of rising infections. 1:55
The importance of getting patients up and out of bed, including those on ventilators when possible, as well as excellent nursing care and other day-to-day supportive care can’t be minimized.
“Supportive care is not the sexy part of it, but it’s so crucial,” Rochwerg said.
It gives patients’ bodies time to heal themselves, he said.
Fear of flood of sick patients
Patty Tamlin, registered nurse working in critical care at a hospital in Toronto’s east end, said she’s also concerned about the coming cold-and-flu season.
“One of the biggest concerns is you may be overrun by patients,” Tamlin said.
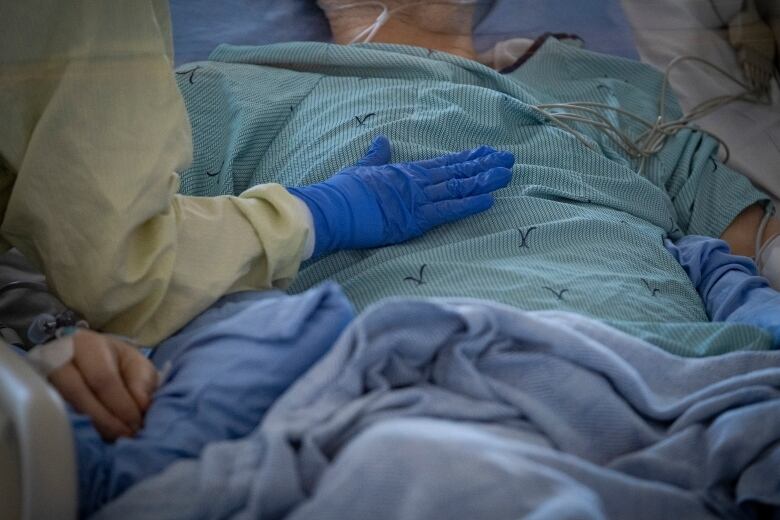
Her message to Canadians? “Tell everyone to get their flu shot.”
In the spring, the Ontario government created more beds for patients needing long-term ventilated care at a rehabilitation hospital. Even if administrators find more space for more beds, adding temp agency nurses can only go so far, she said.
“It’s going to be a long time,” Tamlin said. “It’s fatiguing … to have this constantly on our head all the time about COVID on top of our regular work.”
Experience, though, has helped ICU staff to prepare for a resurgence of COVID-19 patients.
“The more you do something, the more comfortable you are with going in and out of a room,” for example, to perform CPR during a “protected code blue” for cardiac arrest when wearing full personal protective equipment, which can be exhausting. The masks, gowns and gloves need to be donned and removed carefully to avoid health-care workers contaminating themselves.
Dr. Eddy Fan, medical director of the Extracorporeal Life Support (ECLS) program at Toronto’s University Health Network, said the increase in COVID-19 cases so far is “manageable.”
Extracorporeal membrane oxygenation (ECMO) is like an artificial heart and lung machine to support the sickest patients. People with COVID-19 who were intubated at hospitals across Ontario and didn’t improve with conventional therapy were transported to Toronto General for ECMO.
Still, Fan said, “We’re going to need to brace ourselves for another potential flood of very sick patients.”
During the spring, patients were transferred to Toronto General, but family members could not visit. Fan said cutting off patients from their relatives harmed morale not only among loved ones, but it pained people working in the hospital, too.

But influenza season also typically brings patients with lung failure who may need ECMO.
“Their families ask questions like ‘they’re dying of the flu?'” Fan said. “COVID is no different as a viral infection. We see even young patients come with very severe lung failure requiring ECMO.”
During Toronto’s first wave of COVID-19, the team successfully treated a 22-year-old with ECMO.
While respiratory failure from COVID-19 can resemble that of the flu, doctors say the scale is much larger.
Dr. Gregory Haljan, head of Surrey Memorial Hospital’s critical care department in British Columbia, said influenza has vaccines and medical treatments to shorten symptoms and improve death rates. COVID-19 doesn’t, aside from corticosteroids for severe cases.
When Haljan and his co-authors across the Lower Mainland looked at 117 people with COVID-19 who were admitted to ICU between Feb. 20 and April 17, they found the mortality rateranged from one in six to one in 10.
In comparison, the first studies from China and Italy showed mortality rates as high as one in two or one in three.

Safety ‘our primary focus’
Haljan credited having time to prepare, Dr. Bonnie Henry’s “outstanding” leadership as the provincial health officer, the support of British Columbians, hard work and luck.
“We never got overwhelmed,” he said.
To prevent being overwhelmed, Haljan said the hospital and its health region focused on basics, including:
- Engaging patients in the community and long-term care homes through a virtual hospital to keep patients safe at home.
- Improving communication with centralized repositories of information to avoid mixed messages.
- Adapting as the science changes.
“It can be a challenge in that things change very, very slowly because safety is our primary focus,” said Haljan, who works at one of the hospitals caring for among the highest volume of patients in the emergency department, according to the Canadian Institute for Health Information.
“Research is how we keep change safe.”
Haljan said that includes research not only on vaccines and drugs but also measuring patterns and assessing them in areas such as delivering health services.










































Leave a comment