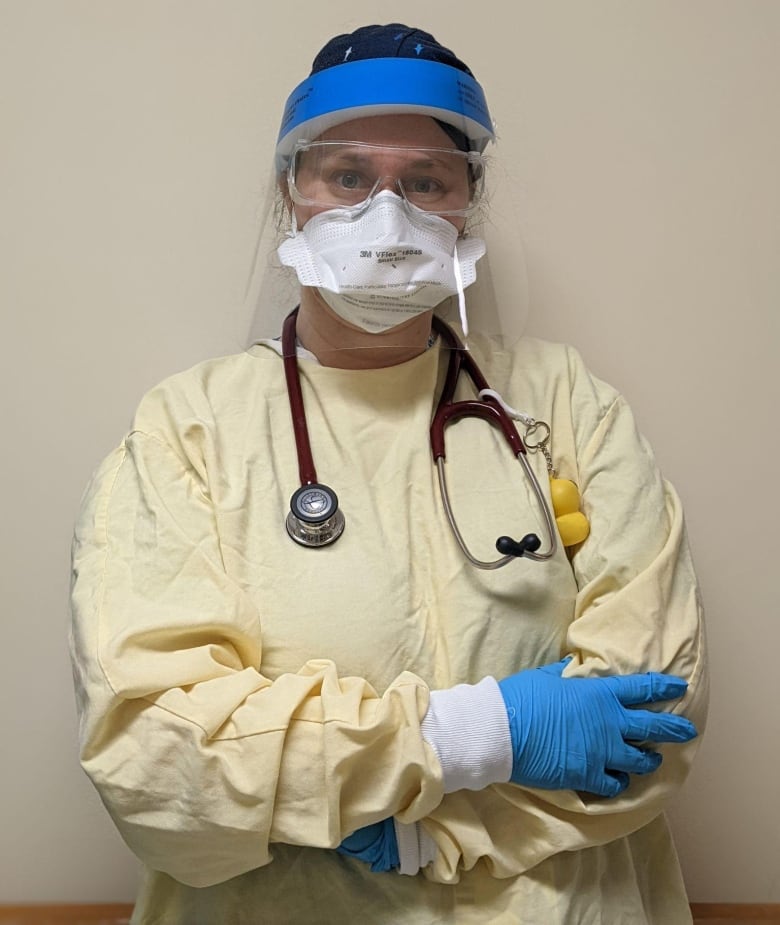
This First Person article is the experience of Dr. Laura Sang, a family physician in the greater Montreal area. For more information about CBC’s First Person stories, please see the FAQ.
WARNING: This article contains references to sexual assault and suicide.
I roll out of bed at 6 a.m., trying not to disturb my sleeping partner. After throwing on a hoodie from the pile of clean clothes I haven’t had time to put away, I fix myself a cup of tea and a bite to eat.
As soon as that first drop of caffeine enters my bloodstream, I open my laptop to review patient charts in preparation for my upcoming clinic.
My inbox has about 20 messages in need of attention from the day before, including one from a secretary stating that my patient — a single mother recently diagnosed with breast cancer — was in distress as her insurance refused to cover her salary while she is off work undergoing chemotherapy treatments. I request the patient be booked during one of my lunch breaks this week to see what can be done to help her out.
Next, I print out a slew of driver’s licence renewal forms for my elderly patients and insurance forms for patients on leave. Each sip of tea is a guilty reminder that I meant to complete these days ago. After a brief “good morning” exchange with my partner at 8 a.m., I drive to work to start my day of actually seeing patients.
At the clinic, I silence my buzzing phone, ignoring the never-ending stream of emails about pandemic precautions, equipment shortage updates and which personnel are out on sick leave as I try to give my full attention to the 18-year-old sobbing in my office. She is struggling to return back to school after being raped.
Her family doesn’t know. I’m the second person she has felt comfortable telling after a teacher refused to give her an extension on her term paper when she sought help.
She stares helplessly into my eyes as she pours her heart out. I feel a growing weight on my shoulders — a sense of responsibility to compensate for a system that has failed her.
Her appointment runs long as I support her through her decision-making process of whether or not to take legal action against the perpetrator.
The remainder of my break is spent calling back patients with urgent lab results and speaking to the nurse from the rehab centre I work at twice a week, trying to manage patients’ hyperglycemia and headaches at a distance.
The last patient walks out my door around 4 p.m. but my workday is far from over. I have a new pile of insurance forms, prescription renewals and specialist referrals to complete.
In my first year as a family doctor, I’m still figuring out the business side of medicine we have to manage. Without sick or vacation days, we only get paid based on our patient interactions. I spend the next two hours trying to finish charting those interactions. All this administrative work — invisible to most — is unpaid.
I spend extra time thoughtfully reworking yet another rejected insurance form so my patient with crippling depression after his son’s suicide will continue to be paid while on leave.
I receive a result from a CT scan showing a brain tumour and try to figure out the fastest way to send the patient to neurosurgery and organize an appointment to discuss the result. After a brief dinner and an hour spent catching up with my partner at home, I skim through all the blood test results that accumulated throughout the day. I struggle to keep my sleeping, fluttering eyes open as I make sure there is nothing urgent before I crawl into bed to do the whole thing all over again the next day. And the next, and the next.
By the time the weekend rolls around (luckily, I am not scheduled to work), I stumble into bed and sleep for about 12 hours.
This schedule reflects the reality of so many family doctors in Quebec. We work and work until we burn out, move to the private sector or leave the field altogether because we simply can no longer bear the weight of our overburdened health-care system.
I feel privileged to do this work. From celebrating a cancer remission to treating depression after a miscarriage, family doctors see patients through many of the defining moments of their lives — moments that many family members aren’t even privy to.
While my work is incredibly rewarding, it is also exhausting. Patient interactions can deeply affect us and it can be hard to find time to process much of the suffering we witness when we are swamped with high patient volumes and paperwork.
And there is often tremendous sacrifice to our personal lives to take care of our patients — postponing dinner plans, missing birthday parties and family reunions. I have had weeks where I didn’t see my partner, because I’m out of the house before he wakes up and home after he has gone to sleep.
This is precisely why it stings every time I see politicians stating that family doctors don’t work hard enough. Asking us to take on more patients as part of reforms to Quebec’s health-care system won’t necessarily improve patient access nor quality of care. The solution is far more complicated.
The next time you feel frustrated that your family doctor is running late, remember we are probably helping someone through a crisis. When we’re only available two days a week, it’s because we are often working in other locations or using unpaid hours to fill out your forms, refer you to specialists and follow up on your lab results.
Remember that we are working for you, even when we don’t see you.
CBC Quebec welcomes your pitches for First Person essays. Please email povquebec@cbc.ca for details.
If you or someone you know is struggling, here’s where to get help:
Support is available for anyone who has been sexually assaulted. You can access crisis lines and local support services through this Government of Canada website or the Ending Violence Association of Canada database. If you’re in immediate danger or fear for your safety or that of others around you, please call 911.










































Leave a comment